Note
Access to this page requires authorization. You can try signing in or changing directories.
Access to this page requires authorization. You can try changing directories.
This reference architecture demonstrates how you can use Microsoft Fabric Real-Time Intelligence to build comprehensive healthcare billing solutions that handle real-time electronic health records (EHR) and revenue cycle management (RCM) data from multiple healthcare sources. You can process continuous healthcare data streams and integrate registration information from Enterprise Resource Planning (ERP) systems to enable intelligent billing anomaly detection, predictive analytics, and automated revenue cycle optimization.
You can manage complex healthcare billing operations where EHR and RCM systems continuously generate data on patient encounters, billing codes, and revenue cycles. The architecture integrates real-time healthcare data through Eventstream processing and maintains comprehensive patient registration information synchronized through Data Factory for unified healthcare billing intelligence and automated deficiency management.
Architecture overview
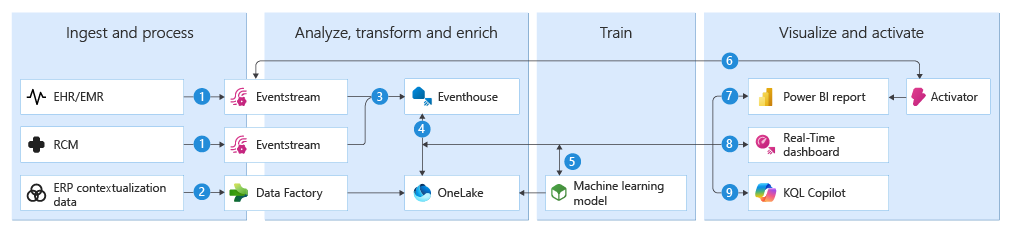
This reference architecture uses Microsoft Fabric Real-Time Intelligence to create a unified platform that processes real-time data from healthcare systems and integrates ERP registration data for intelligent revenue cycle management. You can implement the architecture with four main operational phases: Ingest and process, Analyze, transform and enrich, Train, and Visualize and activate.
Real-time Electronic Health Records (EHR) and Revenue Cycle Management (RCM) data is ingested from multiple sources and processed through Eventstream.
Registration information is synced from Enterprise Resource Planning (ERP) system using Data Factory.
Continuous transformations take place within Eventhouse where Kusto Query Language (KQL) Query queries petabytes of data to detect anomalies like duplicate entries or missing billing codes, and flags them for resolution.
A shortcut is created between Eventhouse and OneLake to link streaming EHR and RCM data with reference ERP data for deeper insights.
Build, train, and score Machine Learning (ML) models in real time, to better predict potential deficiencies and spikes.
Administrators are notified of missing charge code with Activator ahead of a scheduled appointment, which reduces manual intervention and ensures no downstream delays.
Billing managers use Power BI dashboards—connected directly to OneLake and Eventhouse—to monitor reimbursement cycle times and revenue trends.
Real-Time dashboard is used to visualize customized high granularity experience per customer.
Analysts can ask natural language questions by using Copilot.
The following sections explain each operational phase in detail.
Operational phases
Ingest and process
Real-time Electronic Health Records (EHR) and Revenue Cycle Management (RCM) data is ingested from multiple sources and processed through Eventstreams. This continuous data integration captures comprehensive healthcare billing information including:
- Patient encounter data and clinical documentation
- Billing codes, procedures, and diagnostic information
- Insurance claims and authorization data
- Payment processing and reimbursement information
- Provider charges and service documentation
Registration information is synced from ERP using Data Factory, enabling comprehensive patient and provider contextualization including:
- Patient demographics and insurance information
- Provider credentials and billing specifications
- Facility registration and service capabilities
- Insurance contract terms and reimbursement rates
- Regulatory compliance and billing requirements
Real-world scenario example
A large healthcare network processes real-time EHR and RCM data from hundreds of facilities including hospitals, clinics, and specialty practices. Eventstreams ingests millions of patient encounters, billing transactions, and insurance claims daily while Data Factory synchronizes patient registration, insurance eligibility, and provider information from multiple ERP systems to ensure accurate billing and optimal revenue cycle performance.
Analyze, transform, and enrich
Continuous transformations take place within Eventhouse, where KQL Query processes petabytes of streaming data to detect anomalies such as duplicate entries or missing billing codes and flag them for resolution. This real-time processing enables immediate healthcare billing optimization including the following capabilities:
Anomaly detection - Eventhouse continuously identifies duplicate billing entries, missing charge codes, and coding inconsistencies in real time. These anomalies are flagged as they occur, allowing billing teams to correct issues before claims progress further in the revenue cycle.
Data validation - Real-time validation verifies billing accuracy, insurance eligibility, and regulatory compliance across incoming EHR and RCM events. It ensures that only complete and compliant billing data is forwarded to downstream systems and reporting.
Pattern recognition - Revenue cycle trends, reimbursement patterns, and billing performance indicators are detected as they emerge. These insights help healthcare organizations understand operational inefficiencies and optimize reimbursement processes.
Quality assurance - Automated quality checks validate the completeness of clinical documentation and the accuracy of billing codes at scale, reducing the risk of errors that can lead to claim denials or compliance issues.
A shortcut is created between Eventhouse and OneLake to link streaming EHR and RCM data with reference ERP data. This unified data access enables deeper analytical insights across clinical, operational, and financial domains, including the following capabilities:
Real-time healthcare analytics - By correlating clinical and billing data as it arrives, the system provides immediate visibility into revenue optimization opportunities and emerging billing risks.
Patient journey tracking - Linking streaming and reference data creates a comprehensive view of patient encounters and billing progression across healthcare services, from registration through reimbursement.
Provider performance analysis - Real-time tracking of provider billing efficiency and revenue generation, enables data-driven performance management and operational improvements.
Compliance monitoring - Continuous assessment of regulatory compliance and billing standards helps organizations detect potential issues early and maintain adherence to healthcare regulations.
Train
Machine learning models are built, trained, and scored in real time by using Data Science capabilities to predict billing deficiencies, revenue fluctuations, and compliance risks. These models continuously learn from streaming EHR and RCM data combined with historical billing patterns to support proactive revenue cycle optimization.
Billing deficiency prediction - Predictive models identify potential billing errors, missing documentation, and coding deficiencies before claims are submitted. By detecting risks early, healthcare organizations can correct issues upstream and reduce downstream delays and denials.
Revenue spike forecasting - Revenue forecasting models analyze patient volume, service mix, and reimbursement trends to predict revenue spikes and shortfalls. These insights help financial teams plan capacity, staffing, and cash‑flow management more effectively.
Denial prediction analytics - Denial prediction models anticipate insurance claim rejections by analyzing historical denial patterns and real‑time billing attributes. It enables optimization of claim submission strategies and improves overall reimbursement success rates.
Reimbursement optimization - Machine learning models evaluate billing timing, coding scenarios, and payer behavior to recommend optimal reimbursement strategies. These insights support maximum revenue capture while maintaining compliance with payer and regulatory requirements.
Compliance risk modeling - Compliance risk models identify patterns that might indicate regulatory violations or audit exposure. By surfacing risks in real time, organizations can proactively adjust billing practices and reduce the likelihood of compliance issues.
Visualize and activate
Activator in Fabric Real-Time Intelligence notifies administrators of missing charge codes and billing deficiencies ahead of scheduled appointments. With this real-time awareness and automated responses, the system reduces manual intervention and helps prevent downstream delays in the revenue cycle, including the following capabilities:
Proactive billing management - Activator generates automated alerts for missing charge codes, incomplete documentation, and other billing issues before appointment completion. This proactive approach allows healthcare teams to address problems early and avoid costly rework later in the billing process.
Revenue protection - Real-time notifications surface potential revenue loss scenarios as they occur, enabling billing and revenue cycle teams to take corrective action and optimize reimbursement outcomes.
Compliance alerts - Immediate notifications are triggered when regulatory compliance issues or potential audit risks are detected. It helps organizations maintain adherence to healthcare billing standards and respond quickly to emerging compliance concerns.
Workflow optimization - Automated triggers initiated by Activator support continuous billing process improvements by streamlining administrative workflows and reducing operational inefficiencies.
Billing managers use Power BI dashboards connected directly to OneLake and Eventhouse to monitor reimbursement cycle times, billing performance, and revenue trends through unified analytical views, including the following capabilities:
Revenue cycle analytics - Dashboards provide comprehensive visibility into billing performance, collection rates, and reimbursement efficiency across healthcare services and facilities.
Financial performance monitoring - Real-time insights into revenue trends, payment processing, and cash flow help financial leaders make informed decisions and adjust strategies as conditions change.
Operational efficiency analysis - Analytics highlight billing cycle durations, performance of processing claims, and administrative cost drivers, supporting data-driven improvements in revenue cycle operations.
Strategic planning - Long-term revenue forecasting and financial planning are enabled through historical and real-time billing analytics delivered via Power BI.
Real-Time Dashboard visualizes customized and high-granularity experiences tailored to specific healthcare roles and operational needs, providing the following capabilities:
Patient-specific billing views - Dashboards display detailed billing information and payment status for individual patients and encounters, supporting focused resolution of billing issues.
Provider performance dashboards - Real-time visualizations track provider billing efficiency, revenue generation, and compliance metrics to support performance management.
Facility operations monitoring - Dashboards provide facility-level visibility into billing performance and revenue optimization across hospitals, clinics, and specialty practices.
Custom analytics experiences - Customizable dashboard experiences allow organizations to tailor analytics views for different healthcare roles, responsibilities, and decision-making contexts.
By using Copilot, analysts can ask natural language questions, enabling the following capabilities:
Conversational healthcare analytics - Copilot enables billing analysts to ask natural language questions, such as identifying patients with incomplete billing documentation during specific time windows.
Intuitive revenue insights - Natural language queries simplify exploration of complex billing scenarios and revenue trends without requiring deep technical expertise.
Simplified compliance reporting - Analysts can quickly access compliance-related insights and audit preparation information using conversational queries.
Strategic decision support - Conversational access to healthcare billing intelligence supports faster, more informed operational, and strategic decision-making.
Technical benefits and outcomes
The healthcare billing system reference architecture delivers measurable technical and operational benefits by unifying real-time data ingestion, predictive analytics, and automated workflows across EHR, revenue cycle management (RCM), and ERP systems. By enabling continuous insight, proactive intervention, and intelligent automation, the architecture helps healthcare organizations improve billing accuracy, protect revenue, maintain compliance, and optimize operational efficiency at scale.
Healthcare billing intelligence and revenue optimization
This capability focuses on delivering end-to-end visibility into billing operations by continuously analyzing clinical, administrative, and financial data streams. Real-time intelligence and predictive analytics enable early detection of revenue risks, improve reimbursement outcomes, and provide a consolidated view of billing performance across facilities and services.
Real-time billing monitoring enables continuous analysis of EHR and RCM events to detect billing deficiencies as they occur. This immediate visibility allows organizations to address missing charge codes, duplicate entries, and coding inconsistencies before they impact downstream reimbursement.
Predictive analytics extend this capability by using machine learning models to forecast billing issues and revenue cycle risks. These models help healthcare organizations proactively optimize reimbursement rates and improve overall billing performance.
Unified healthcare platform - By integrating real-time billing data with patient registration and reference data, the architecture provides a unified healthcare platform. This consolidated view supports comprehensive billing intelligence across facilities, providers, and services.
Anomaly detection capabilities further enhance revenue protection by identifying billing errors and inconsistencies in real time. Early detection reduces rework, minimizes claim denials, and improves cash flow.
Automated healthcare operations
Automated healthcare operations streamline billing workflows and reduce manual intervention through real-time alerts, rule-based triggers, and predictive insights. By embedding automation directly into billing and compliance processes, organizations can respond faster to issues, improve consistency, and reduce operational overhead.
Intelligent billing alerts deliver real-time notifications for billing deficiencies, missing charge codes, and compliance issues. These alerts ensure that administrators and billing teams are informed immediately when action is required.
Automated revenue workflows use triggers and rules to streamline billing processes such as claim preparation, submission, and payment processing. Automation reduces manual effort and improves operational consistency.
Proactive billing management is enabled through predictive models that surface risks before billing issues materialize. This proactive approach improves billing efficiency and protects revenue by addressing problems upstream.
Dynamic compliance monitoring allows organizations to adjust billing processes in real time as regulatory conditions change. Continuous assessment supports sustained adherence to healthcare billing standards.
Advanced analytics and business intelligence
Advanced analytics and business intelligence capabilities transform real-time and historical billing data into actionable insights. By correlating data across clinical, operational, and financial systems, organizations gain deeper visibility into revenue performance, compliance trends, and enterprise-wide operational health.
Real-time healthcare analytics correlate clinical and billing data to deliver immediate insights into revenue optimization and compliance performance. Organizations can respond quickly to emerging trends and operational changes.
Cross-system intelligence provides deep business intelligence across healthcare facilities and provider networks. Comprehensive reports aggregate revenue cycle data to support enterprise‑wide performance analysis.
Natural language processing capabilities enable conversational access to complex billing scenarios. Analysts can explore data using intuitive queries without requiring advanced technical skills.
Predictive and historical analysis combines real-time streaming data with historical billing patterns. This integrated approach supports informed decision‑making across short‑term operations and long‑term financial planning.
Cost optimization and operational efficiency
This set of capabilities focuses on reducing administrative costs while improving billing accuracy and revenue cycle performance. Predictive insights, automated validation, and data-driven decision support help organizations minimize rework, reduce claim denials, and align operational improvements with long-term financial and compliance goals.
Predictive cost management reduces administrative overhead by identifying billing errors early and minimizing manual correction efforts. Machine learning–driven predictions help organizations control operational costs.
Revenue cycle efficiency is improved by maximizing reimbursement rates and reducing claim denials through continuous monitoring and predictive analytics. Faster, more accurate billing processes shorten reimbursement cycle times.
Billing optimization ensures higher accuracy and stronger compliance through automated validation and quality assurance mechanisms. These capabilities improve consistency across billing operations.
Strategic decision support enables data‑driven planning for revenue cycle improvements and compliance management. Technical insights derived from real-time and historical data support long‑term operational and financial strategies.
Implementation considerations
Implementing a real-time healthcare billing system requires deliberate planning across data architecture, security, integration, observability, and cost governance. These considerations help ensure that the solution scales reliably with patient volumes, maintains regulatory compliance, delivers consistent low‑latency performance, and operates within sustainable cost boundaries.
Data architecture requirements
A robust data architecture is foundational to delivering reliable real-time billing intelligence. The platform must support high‑volume data ingestion, low‑latency processing, strong data validation, and long‑term scalability while maintaining resilience across interconnected healthcare systems.
High-throughput ingestion is essential to support real-time EHR and RCM data from multiple healthcare destinations. The architecture should be designed to handle burst capacity during peak patient volumes without data loss or latency degradation.
Real-time processing requirements demand immediate responsiveness for critical billing alerts. Systems should be designed to deliver sub–two-second responses for billing updates and near‑instant processing for deficiency predictions and anomaly detection.
Data quality and validation are foundational to reliable billing outcomes. Real-time validation should be implemented for patient identification, billing code accuracy, insurance eligibility, and compliance calculations, with mechanisms for automated error detection and correction.
Scalability planning ensures the architecture can grow alongside healthcare networks. The platform should accommodate increasing patient volumes, expanded provider networks, and evolving regulatory requirements without major rearchitecture.
Storage requirements must account for real-time events, historical billing records, and compliance documentation. Retention policies should balance analytical needs with regulatory requirements and cost efficiency.
Healthcare system integration should be seamless and resilient. The architecture must support continuous connectivity with EHR systems, RCM platforms, and ERP registration systems to maintain consistent and accurate billing intelligence.
Security and compliance
Healthcare billing systems handle highly sensitive patient and financial data, making security and regulatory compliance critical design requirements. Strong access controls, comprehensive auditing, and consistent privacy enforcement help protect patient data, satisfy regulatory mandates, and maintain trust across clinical and administrative stakeholders.
Access controls should enforce role-based permissions aligned with healthcare responsibilities, including billing administrators, clinical staff, revenue cycle managers, and compliance officers. Multifactor authentication and privileged access management are essential for securing administrative functions.
Audit trails must capture all patient data access, billing activities, and revenue cycle operations. Comprehensive, immutable logging supports regulatory compliance, audit readiness, and automated compliance reporting.
Data privacy protections must ensure compliance with HIPAA and other healthcare regulations. Safeguards should be applied consistently across EHR data, billing records, and analytical outputs to maintain patient trust and regulatory adherence.
Integration points
Effective billing intelligence depends on seamless integration across clinical, financial, and operational systems. Clearly defined integration points ensure consistent data flow between internal healthcare platforms and external services, enabling accurate, real‑time billing operations and downstream analytics.
Electronic health record (EHR) systems provide clinical data and patient encounter information that drives downstream billing and analytics workflows.
Revenue cycle management (RCM) platforms integrate in real time to support billing, claims submission, and payment processing activities.
Enterprise resource planning (ERP) systems synchronize patient registration data, insurance information, and provider metadata that enrich billing intelligence.
External data sources, including insurance providers, regulatory systems, payment processors, and healthcare information exchanges, contribute validation, authorization, and reimbursement context through secure APIs.
Monitoring and observability
Continuous monitoring and observability are essential to maintaining reliability in real-time billing workflows. Proactive visibility into system health, data quality, and performance metrics allows organizations to detect issues early, maintain service‑level objectives, and ensure uninterrupted billing operations.
Operational monitoring provides real-time visibility into system health across data ingestion, Eventhouse processing, and Activator notifications. Automated alerts surface system anomalies and performance degradations as they occur.
Data quality monitoring continuously validates incoming healthcare data. Alerts are generated for communication failures, invalid billing codes, and corrupted patient information to prevent downstream impact.
Performance metrics track ingestion latency, query response times, and machine learning model accuracy. Service-level objectives and SLA monitoring help ensure consistent system reliability.
Cost optimization
Cost optimization ensures that real-time billing architectures remain financially sustainable at scale. By aligning capacity, data retention, and operational insights with healthcare demand patterns, organizations can control infrastructure costs while maximizing the efficiency and value of revenue cycle operations.
Capacity management ensures Fabric resources are sized appropriately based on healthcare network scale and data volume. Autoscaling supports peak patient volumes, while optimization strategies reduce costs during low‑activity periods.
Data lifecycle management automates archival of older healthcare data to lower‑cost storage tiers. Retention policies align with regulatory mandates, and nonessential billing data is deleted to control storage costs.
Revenue cycle cost optimization correlates billing performance patterns with operational expenses. Real-time insights help minimize administrative overhead while maximizing revenue capture.
Next steps
The following phased approach helps healthcare organizations move from initial planning to validated, production‑ready deployment of a real-time billing system. By progressing incrementally, teams can reduce implementation risk, validate performance at each stage, and ensure alignment with clinical, billing, and compliance requirements.
Phase 1: Foundation setup
This phase focuses on establishing the core technical foundation for real-time healthcare billing intelligence. Activities in this stage emphasize platform readiness, capacity planning, data ingestion design, and baseline analytics to support reliable, low‑latency billing workflows.
Review Fabric Real-Time Intelligence capabilities, and understand capacity requirements for your healthcare billing scale (EHR systems, patient volumes, and billing complexity).
Plan your Eventstream integration strategy for EHR and RCM data ingestion. Start with critical billing processes and high-volume patient services.
Design your real-time analytics implementation in Eventhouse for processing healthcare events with immediate response requirements.
Configure OneLake for healthcare reference data and historical billing analytics with appropriate retention policies.
Phase 2: Pilot implementation
The pilot phase enables organizations to validate the architecture in a controlled environment using real healthcare data and representative billing scenarios. By limiting scope to selected facilities and processes, teams can test integrations, refine analytics, and confirm that billing insights and alerts meet operational needs.
Start with a subset of healthcare facilities and billing processes to validate the architecture and integration performance.
Implement core data flows for billing monitoring, anomaly detection, and basic alerting capabilities.
Establish integration with EHR, RCM, and ERP systems for comprehensive healthcare billing visibility.
Deploy Real-Time Dashboard for billing monitoring with customized high granularity experiences for different healthcare roles.
Phase 3: Operational validation
Operational validation ensures the solution is resilient, compliant, and ready for enterprise-scale use. This phase focuses on stress testing, alert accuracy, regulatory adherence, and user readiness to confirm that the system can support sustained, real‑time billing operations in production environments.
Test system performance during peak patient volume periods and billing cycle stress scenarios.
Validate Activator rules for billing deficiency alerts and compliance violation management.
Ensure compliance with HIPAA regulations and healthcare billing standards.
Train your healthcare teams on dashboard usage, alert management, and natural language analytics for billing optimization.
Advanced implementation
Advanced implementation builds on the foundational and validated phases to deliver intelligent, scalable, and AI‑driven healthcare billing capabilities. This stage focuses on embedding machine learning, automation, and conversational analytics into billing operations while scaling the architecture to support enterprise‑wide healthcare networks and advanced decision‑making needs.
Intelligent automation and AI
Intelligent automation and AI extend real‑time billing intelligence by introducing predictive models, automated decisioning, and natural language analytics. These capabilities enable healthcare organizations to proactively manage revenue risks, optimize billing performance, and support operational decisions through real‑time, data‑driven insights.
Set up advanced Data Science capabilities for building, training, and scoring predictive ML models for billing optimization and revenue forecasting.
Implement Activator for sophisticated healthcare automation including predictive billing management, dynamic revenue optimization, and automated compliance monitoring.
Deploy Copilot for natural language analytics enabling healthcare teams to query complex billing scenarios using conversational interfaces.
Create intelligent healthcare billing systems that provide real-time decision support based on patient data, billing performance, and compliance requirements.
Enterprise-scale deployment
Enterprise‑scale deployment ensures the billing architecture supports large, distributed healthcare networks with consistent performance, visibility, and governance. By centralizing analytics, dashboards, and machine learning capabilities, organizations can optimize revenue and compliance across facilities while supporting executive‑level reporting and strategic planning.
Scale to full healthcare network operations with comprehensive billing coverage and centralized monitoring across all facilities and providers.
Implement advanced analytics for cross-facility revenue optimization, compliance management, and billing performance analysis.
Create comprehensive dashboards with Power BI direct query capabilities and Real-Time Dashboard for executive reporting, operational monitoring, and regulatory compliance.
Develop enterprise-grade machine learning models for revenue prediction, billing optimization, and healthcare network expansion planning.
Related resources
- Real-Time Intelligence documentation
- Activator for automated alerting
- Eventstreams for real-time data ingestion
- Healthcare data analytics with Microsoft Fabric
- Advanced analytics and machine learning
- Microsoft Fabric Real-Time Intelligence capacity planning
- OneLake data storage overview
- Data Factory for data integration